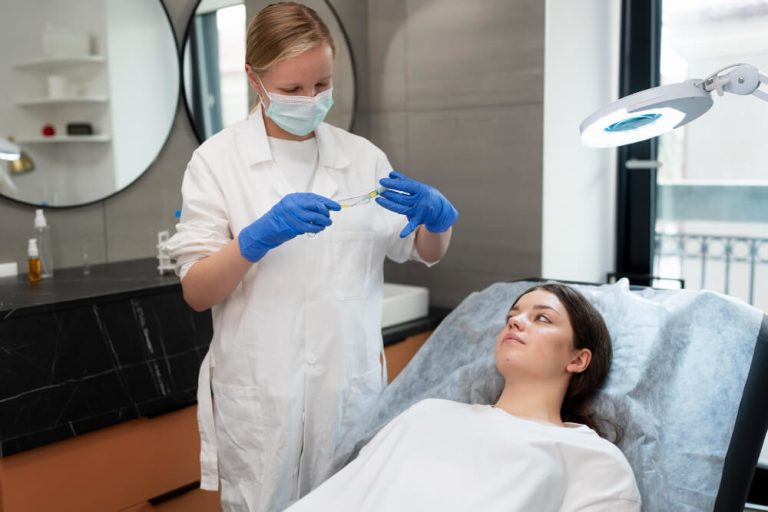
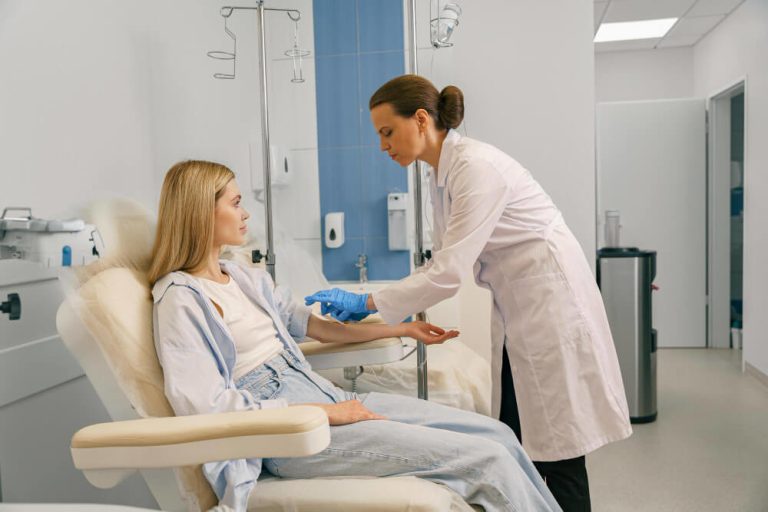
Andropause Training: Your Ultimate Guide to Thriving in Midlife and Beyond
For many men, the years after 40 bring about subtle yet undeniable shifts. Energy levels may dip, workouts feel harder, and a certain mental sharpness seems to fade. This experience, often silently endured, has a name: andropause. It’s a natural phase of aging characterized by a gradual decline in hormones, most notably testosterone.
While this transition is a normal part of life, it doesn’t mean you have to accept a diminished sense of vitality as your new reality. The key to navigating this stage successfully lies in a proactive, holistic approach. This is where a comprehensive strategy involving targeted lifestyle modifications becomes essential, a concept expertly covered in specialized Andropause training programs designed for health practitioners.
This is not about finding a mythical fountain of youth, but about understanding the changes your body is undergoing and giving it the precise tools it needs to adapt and thrive. Through a combination of smart exercise, strategic nutrition, and supportive lifestyle habits, you can effectively manage the symptoms of andropause and reclaim your strength, energy, and focus for years to come.
What Exactly is Andropause?
Unlike female menopause, which involves a rapid and definitive drop in hormones, andropause is a much more gradual process. Often referred to as male menopause, late-onset hypogonadism, or androgen deficiency, it describes the age-related decline in testosterone and other androgens like dehydroepiandrosterone (DHEA) in men.
This decline typically begins in a man’s 30s, with testosterone levels decreasing by about 1% per year. While this slow trickle may not be noticeable at first, the cumulative effect can lead to significant symptoms by the time a man reaches his late 40s, 50s, or 60s. The onset and severity of these symptoms can vary widely, influenced by genetics, diet, stress levels, and overall health.
It’s crucial to understand that andropause is not a disease but a biological transition. However, its symptoms can significantly impact one’s quality of life. Recognizing this allows for a shift from passive acceptance to active management, empowering men to take control of their health during this important life stage.
What are the Common Signs and Symptoms of Andropause?
The effects of declining androgens are systemic, meaning they can appear in various aspects of your physical, mental, and emotional well-being. Recognizing these signs is the first step toward addressing them effectively. The symptoms are often interconnected, creating a cascade effect that can impact daily life.

How Do Physical Symptoms Manifest?
Physically, one of the most common complaints is a persistent feeling of fatigue or a general lack of energy that isn’t resolved with a good night’s sleep. Many men notice a change in their body composition; muscle mass becomes harder to build and maintain, a condition known as sarcopenia. Simultaneously, body fat, particularly around the abdomen, tends to increase.
Other physical signs include a reduction in bone density, which can increase the risk of osteoporosis and fractures. Some men may also experience hair loss on the body and head, dry skin, and an increased need for recovery time after physical exertion. These changes are a direct result of lower testosterone levels, which play a vital role in maintaining muscle, bone, and metabolic health.

What Are the Emotional and Cognitive Changes?
The hormonal shifts of andropause extend beyond the physical. Many men report changes in their mood, including increased irritability, sadness, or a general lack of motivation. That ‘get up and go’ feeling can be replaced by a sense of apathy or listlessness.
Cognitive function can also be affected. ‘Brain fog’ is a frequent complaint, describing difficulty with concentration, memory recall, and mental clarity. These emotional and cognitive symptoms can be particularly frustrating, impacting work performance, personal relationships, and overall enjoyment of life.
How Does Andropause Affect Sexual Health?
Testosterone is a primary driver of male libido, so a decline in this hormone often leads to a decreased interest in sex. Beyond desire, physical performance can also be affected. Erectile dysfunction, or the inability to achieve or maintain an erection firm enough for intercourse, becomes more common.
Men might also notice a reduction in the frequency of spontaneous morning erections, which is another indicator of lower testosterone levels. These changes in sexual function can be a significant source of stress and can affect self-esteem and intimate relationships, making them an important aspect of andropause to address.

Why is ‘Training’ the Key to Managing Andropause?
The term ‘training’ in the context of andropause goes far beyond simply hitting the gym. It represents a comprehensive and intentional strategy to retrain your body and lifestyle to counteract the effects of hormonal decline. It is a multi-faceted approach that integrates targeted exercise, precision nutrition, stress mitigation, and sleep optimization.
This holistic view is powerful because the pillars of health are deeply interconnected. Poor sleep elevates stress hormones that suppress testosterone. A nutrient-poor diet robs your body of the building blocks for hormone production. A sedentary lifestyle accelerates muscle and bone loss. Andropause training addresses all these factors simultaneously.
By adopting a structured training plan, you are not just treating symptoms; you are addressing the root causes and creating an internal environment that supports hormonal balance and vitality. This proactive stance is the most effective way to manage andropause and build a foundation for long-term health and wellness.

What is the Best Exercise Regimen for Andropause?
A well-rounded exercise program is the cornerstone of any effective andropause management plan. The right kind of physical activity can directly boost testosterone, improve body composition, elevate mood, and protect against age-related diseases. The ideal regimen combines strength training, cardiovascular work, and mobility.

Why is Strength Training Non-Negotiable?
If you could only choose one form of exercise to combat andropause, it should be resistance training. Lifting weights, especially with compound movements that engage multiple muscle groups, sends a powerful signal to your body to produce more testosterone. Exercises like squats, deadlifts, bench presses, and overhead presses are incredibly effective.
This type of training directly counteracts sarcopenia by stimulating muscle protein synthesis, helping you build and preserve lean mass. More muscle means a higher resting metabolic rate, which makes it easier to manage body fat. Furthermore, the stress that weight-bearing exercise places on your bones stimulates them to become denser and stronger. For guidance, many resources outline the best workouts for men over 40 to help you get started safely and effectively.

How Does Cardiovascular Exercise Fit In?
While strength training builds the engine, cardiovascular exercise keeps it running smoothly. Cardio is essential for heart health, helping to lower blood pressure, improve cholesterol profiles, and enhance circulation. It’s also a fantastic tool for managing weight and reducing visceral fat, the dangerous type of fat that surrounds your organs.
A balanced approach includes both high-intensity interval training (HIIT) and moderate-intensity steady-state cardio. HIIT involves short bursts of all-out effort followed by brief recovery periods, which can be a potent stimulus for hormone production and fat loss. Steady-state cardio, like brisk walking, cycling, or swimming, is excellent for building endurance and aiding recovery. The key is to find a routine that works for you, as consistency is paramount for any exercise for men at every age.

Should Flexibility and Mobility Be a Priority?
As we age, joints can become stiff and range of motion can decrease, which increases the risk of injury and can make daily activities more difficult. Neglecting flexibility and mobility is a common mistake. Incorporating practices like dynamic stretching before workouts, static stretching after, and even yoga or Pilates can make a world of difference.
Improved mobility not only helps prevent injuries but also allows you to perform strength training exercises with better form, leading to better results. It reduces aches and pains, improves posture, and contributes to an overall feeling of physical freedom and capability. For a population that is getting older, finding the best exercises for men over 50 often includes a significant focus on maintaining this flexibility.
How Does Nutrition Support Andropause Training?
Exercise creates the stimulus for change, but nutrition provides the raw materials. You cannot out-train a poor diet, especially when your goal is to optimize hormonal health. Strategic nutrition for andropause focuses on providing the body with the building blocks for testosterone, managing blood sugar, and reducing inflammation.
What Macronutrients Should You Focus On?
Protein is paramount. It provides the amino acids necessary to repair and build muscle tissue after your workouts. Aim for a consistent intake of high-quality protein from sources like lean meats, poultry, fish, eggs, and legumes throughout the day.
Healthy fats are also critical, as cholesterol is the precursor molecule from which testosterone is synthesized. Don’t be afraid of fats from sources like avocados, nuts, seeds, olive oil, and fatty fish. These fats support hormone production and reduce inflammation.
Complex carbohydrates, such as those from vegetables, whole grains, and legumes, provide the sustained energy needed to fuel workouts and daily activities. They are preferable to simple sugars, which can spike insulin and negatively impact hormone balance.

Are There Specific Micronutrients That Help?
Several vitamins and minerals play a direct role in testosterone production and overall health. Zinc is a key player; a deficiency is strongly linked to low testosterone. Oysters, red meat, and pumpkin seeds are excellent sources.
Magnesium is another vital mineral that is involved in hundreds of bodily processes, including muscle function and energy production. It has also been shown to support healthy testosterone levels. Look for it in leafy greens, nuts, and dark chocolate.
Vitamin D, often called the ‘sunshine vitamin’, functions more like a hormone in the body and is essential for both testosterone production and bone health. If you don’t get regular sun exposure, supplementation is often necessary.

What Lifestyle Factors Complement Physical Training?
Your efforts in the gym and kitchen can be amplified or undermined by your daily habits. Optimizing your lifestyle, particularly in the areas of sleep and stress management, is a non-negotiable part of a successful andropause strategy.

Why is Sleep the Ultimate Recovery Tool?
Sleep is when your body does most of its repair and hormone production. The majority of your daily testosterone release occurs during sleep. Consistently skimping on sleep, or having poor quality sleep, directly suppresses testosterone levels and elevates the stress hormone cortisol.
Aim for 7 to 9 hours of quality sleep per night. Improve your sleep hygiene by creating a dark, cool, and quiet bedroom environment. Avoid screens for at least an hour before bed, establish a consistent sleep schedule, and limit caffeine and alcohol, especially in the evening.
How Can You Manage Stress to Improve Hormones?
Chronic stress is a major enemy of hormonal health. When you’re constantly stressed, your body produces high levels of cortisol. Cortisol and testosterone have an inverse relationship; when one is high, the other tends to be low. High cortisol can block testosterone’s effects and encourage the storage of abdominal fat.
Incorporate stress-management techniques into your daily routine. This could include mindfulness meditation, deep-breathing exercises, journaling, or spending time in nature. Making time for hobbies and social connections that you enjoy is also a powerful way to de-stress and support your overall well-being.

When Should You Consider Medical Support?
Lifestyle interventions form the powerful foundation of andropause management. For many men, a dedicated approach to training, nutrition, sleep, and stress is enough to significantly improve symptoms and quality of life. However, for some, these changes may not be sufficient on their own.
If you’ve implemented these strategies and are still struggling, it may be time to seek professional medical advice. A healthcare provider specializing in hormone health can run blood tests to get a clear picture of your hormone levels and rule out other potential medical issues. A formal diagnosis of a condition like hypogonadism requires this level of clinical investigation.
Working with a knowledgeable practitioner is crucial. They will operate according to established clinical guidelines for treating andropause to ensure your care is both safe and effective. If medical treatment is deemed appropriate, it’s often more complex than a simple prescription.
For instance, Testosterone Replacement Therapy (TRT) is a potential treatment, but it requires careful management. Professionals use advanced TRT dosing and monitoring protocols to tailor treatment to the individual, minimizing side effects and maximizing benefits. It’s also important to be aware that providers must navigate a complex legal and regulatory landscape of anti-aging medicine to provide these specialized services.
Andropause is not an endpoint but a turning point. It’s an opportunity to become more intentional about your health than ever before. By embracing a holistic training approach that encompasses exercise, nutrition, and lifestyle, you can effectively manage its symptoms and build a stronger, more resilient, and more vital version of yourself for the decades ahead.
Frequently Asked Questions

How do I know if my symptoms are from andropause or just normal aging?
Distinguishing between andropause and the natural aging process can be challenging because their symptoms, such as fatigue and decreased libido, often overlap. The key difference lies in a clinically significant drop in testosterone levels, which must be confirmed through medical testing. A primary care provider will assess the severity and combination of your symptoms, rather than attributing them solely to your age, to determine if a hormonal evaluation is necessary.
The diagnostic process involves a thorough consultation and specific blood tests, typically performed in the morning when testosterone levels are highest. Your doctor will likely test your total and free testosterone on at least two separate occasions to confirm a consistently low level. They will also work to rule out other medical conditions that could be causing your symptoms, ensuring an accurate diagnosis of late-onset hypogonadism before discussing management options.

Can lifestyle changes alone be enough to manage andropause symptoms?
For men with mild symptoms or testosterone levels on the lower end of the normal range, targeted lifestyle modifications can be highly effective and sometimes sufficient. Engaging in regular resistance training, maintaining a healthy weight, and ensuring a balanced diet rich in nutrients like zinc and vitamin D can naturally support hormone production. Improving sleep quality and managing stress are also crucial strategies that can boost energy, improve mood, and positively impact overall well-being.
However, for individuals with a confirmed diagnosis of late-onset hypogonadism and more significant symptoms, lifestyle changes are typically considered a vital component of a broader treatment plan, not a standalone cure. While these positive habits are essential for maximizing the benefits of any medical intervention and supporting overall health, they may not be able to raise testosterone levels enough to resolve moderate to severe symptoms on their own. Your physician will help you create an integrated plan that addresses your specific needs.

What are the main risks associated with Testosterone Replacement Therapy (TRT) and how are they monitored?
While TRT can be highly effective, it is not without potential risks that require careful consideration and management. Common side effects can include acne, fluid retention, and an increase in red blood cell count (erythrocytosis), which can elevate the risk of blood clots. There is also ongoing research into the long-term effects of TRT on prostate health and cardiovascular events, making a thorough initial risk assessment by your doctor essential.
To ensure patient safety, primary care providers implement a strict monitoring protocol for anyone undergoing TRT. This involves regular follow-up appointments and blood tests to check testosterone levels, hematocrit (red blood cell concentration), and prostate-specific antigen (PSA). This continuous monitoring allows your doctor to adjust your dosage as needed and proactively manage any side effects, ensuring the benefits of the therapy continue to outweigh the risks.
Discover the most comprehensive functional medicine training, longevity training, and biohacking certification programs designed specifically for healthcare professionals, medics, and clinic owners who want to master regenerative medicine protocols and anti-aging therapies. Elevate your practice with Talking Longevity.